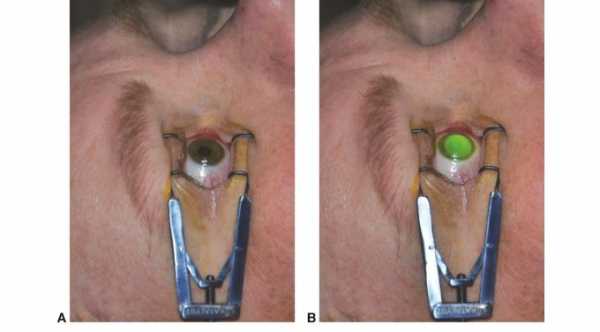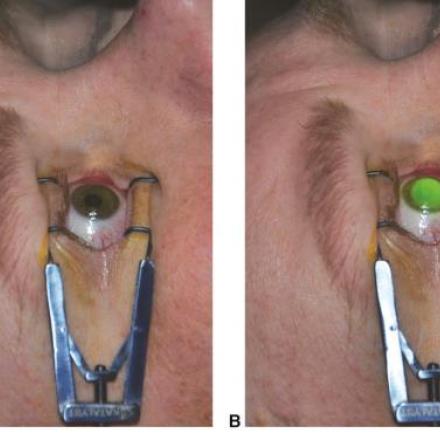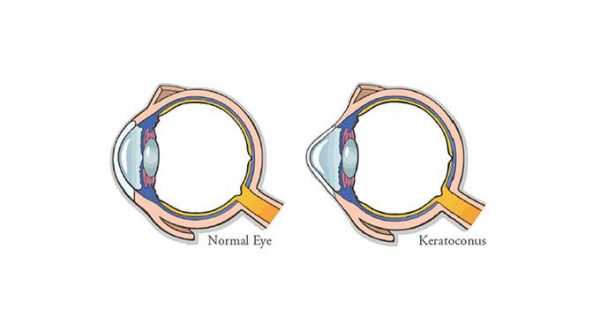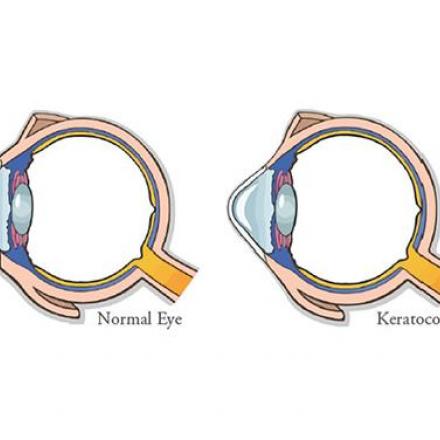
Treatment of Keratoconus depends on the severity of the condition
1- Corneal Collagen Cross linking c3
Patients with good vision at presentation should be treated with corneal collage cross linking procedure with Riboflavin eye drops. This procedure with stabilize the cornea and prevent it from change its shape. It will do that by increasing the cross linking between the collages.
By this step your eye doctor will ensure that your vision will not deteriorate and your condition will not progress with time. It can be done also for patients with iatrogenic keratoconus or ectasia and also after corneal rings implants. Read more about Corneal Collagen Cross Linking.
2- Treatment of the risk factors
The next step will be to eliminate the risk factors such as eye rubbing from allergic conditions, chronic eye irritation or poor fitted contact lens.
3- Eyeglasses
This is usually the first line of treatment. Not all patients will be improved with this step. You have to know that eye glasses will not step the progressive of keratoconus.
4- Contact Lenses for Keratoconus
Which can be either soft contact lens for patients with mild keratoconus or hard contact lenses which can be used for more advanced condition. The hard smooth surface of the hard contact lens will eliminate the irregular shape of the cornea and this will help to focus the lights to one spot.
Not all patients will be improved with this step. You have to know that both eyeglasses and contact lenses will not stop the progression of keratoconus. Only cross linking can do so.
Contact Lenses for Keratoconus are:
1- Gas Permeable Contact Lenses
2- Hybrid Contact Lenses
3- Scleral Contact Lenses
5- Intracorneal Rings
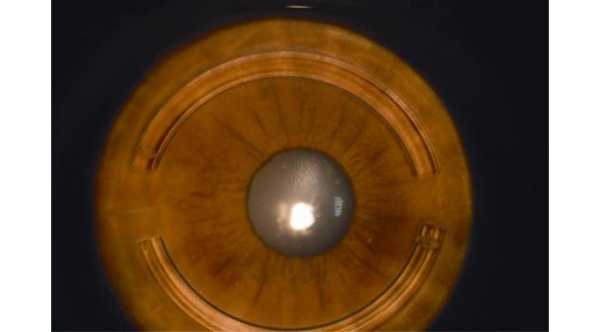
This procedure received approval from FDA for keratoconus treatment. In this procedure, a special ring such as intacs will be implanted inside the cornea. These implanted rings change the conical shape of the cornea to more regular one.
Also not all patients will be improved with this procedure. These rings have the advantages of being removable and exchangeable with minimum complications.
This procedure can’t prevent the progression of the keratoconus but it can delay or slow the progression of it. Sometimes, your eye doctor will do corneal rings, and if you are happy with your vision, he can do cross linking to stabilize the cornea.
6- Corneal Transplant
This procedure can be done for patients who have severe conical shaped keratoconus and who didn’t show any improvement with the previous measurements. It can be done also for patients with corneal scars due to hydrops.
7- New Keratoconus treatment with pachymetry assisted laser keratoplasty
Some corneal disease such as keratoconus and corneal dystrophy can cause scar and opacity in the anterior part of the cornea while leaving the posterior part and Descement’s membrane of the cornea clear and in this case it would be greta just to treat the anterior part while leaving the unaffected posterior part in a procedure called Lamellar Keratoplasty. In this procedure the affected anterior part of the cornea is replaced with a donor corneal graft.
There are many advantages of lamellar keratoplasty over the traditional penetrating keratoplasty such as:
1- Faster visual rehabilitation.
2- Reduce the incidence of post operation astigmatism.
3- Reduce the risk of corneal graft rejection especially endothelial rejection.
4- In Lamellar Keratoplasty there is no invasion of the anterior chamber as penetrating Keratoplasty and this help to reduce the incidence of intraoperative complications that results from penetrating the eye such as endophthalmitis, cataract and glaucoma.
The disadvantage of this procedure is that the interface between the donor tissue and host corneal bed can develop opacities and haziness which can cause irregular astigmatism and decrease the final visual acuity.
Lamellar Keratoplasty can be done with excimer laser ablation which provide high degree of accuracy. Laser ablation is guided by pachymetry and this new procedure is called Pachymetry assisted laser keratoplasty (PALK).
In this procedure, the desirable diameter and thickness of the scared anterior part of the cornea (should be less than 300 microns in depth) that we want to remove can be obtained by using excimer laser that is guided by automatic pachymetry.
Pachymetry provides a map of the thickness of the whole cornea and helps the surgeon to measure the exact depth of scared tissue, obtain uniform and even thickness of ablation and avoid microperforation into the anterior chamber that mainly happen accidently in manual lamellar Keratoplasty.
The created flap is removed and the donor corneal tissue is placed on the host corneal bed and sutures are applied. Patients who underwent this procedure had faster visual recovery and had less post operative astigmatism.
In a study, this procedure can be used as new keratoconus treatment to treat moderate to severe keratoconus instead of using the traditional penetrating Keratoplasty. They found that the visual recovery was faster for patients who underwent this procedure and the best corrected vision after the procedure was better.