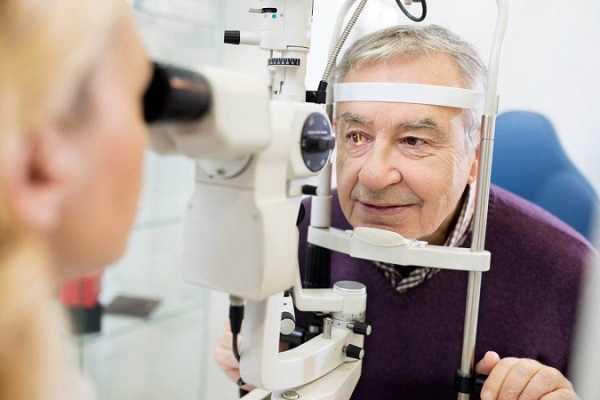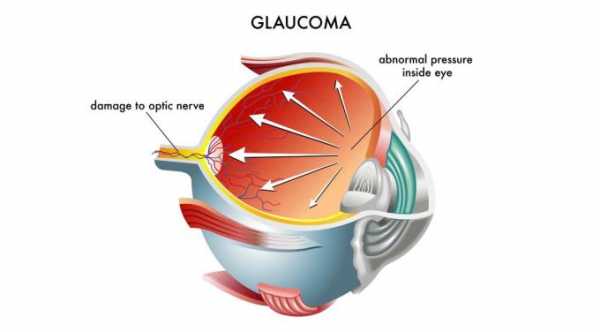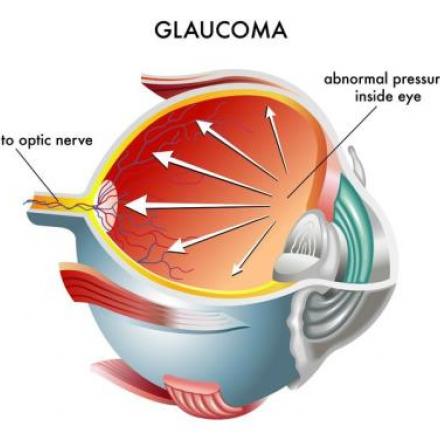
ABiC Glaucoma Procedure
Ab Interno Canaloplasty or ABiC is aminimally-invasive Glaucoma Surgery (MIGS) procedure that is based on the same principles of angioplasty which is used to widen blocked coronary arteries.
Minimally invasive glaucoma surgeries or MIGS are highly effective, low risk surgical procedures that reduce intraocular pressure and/or medications with a safety profile that is better than that of the older, more aggressive glaucoma surgical procedures such as trabeculectomy or tube shunt.
Minimally invasive glaucoma surgeries work by enhancing aqueous humor filtration through natural outflow systems of the eye.
ABiC is an FDA-approved procedure performed to control the intraocular pressure (IOP) without damaging tissues and without the placement of permanent implants in the eye.
Features of iTrack microcatheter of ABiC?
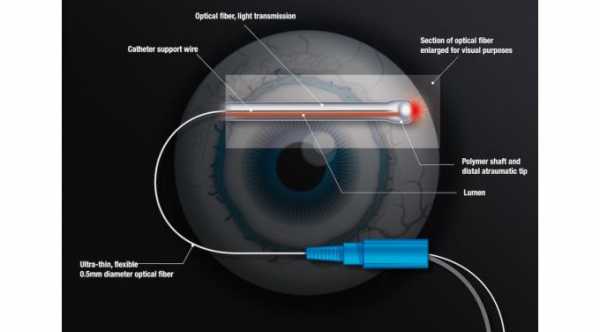
ABiC uses an illuminated microcatheter technology called iTrack to viscodilate the Schlemm channels of the eye in order to improve aqueous outflow without a stent or shunt. Instead of changing or bypassing the natural drainage pathways of aqueous humor, ABiC is designed to restore the natural outflow pathway by addressing all drainage channels.
The coating of the iTrack microcatheter allows it to glide easily through the Schlemm canal. The light at the tip of the microcatheter allows easy visualization of the catheter at all times. The microcatheter is long enough to allow 360° of treatment and also to allow to use it in the opposite direction in case there is a blockage within Schlemm Canal in one direction.
The iTrack microcatheter permits control of viscoelastic infusion in which you can infuse more viscoelastic to achieve better expansion and dilation of the canal especially in areas with blockage of adhesions.
The difference between ABiC and Canaloplasty
The traditional canaloplasty requires large conjunctival dissections and scleral flap with the insertion of a tension suture in the Schlemm Canal. By contrast, ABiC causes less damage to the eye because there is no conjunctival dissection and there is no need for the creation of scleral flap. These things help to reduce both surgical (The procedure can take up to 10-15 minutes) and recovery times. In canaloplasty the procedure might take up to 1 hour.
Another important difference is that ABiC can be performed easily in patients who had failed surgical procedures from trabeculectomies and tube shunt as there is no need for further conjunctival and scleral flap dissections.
Despite the differences between these two procedures both of them are very effective in the reduction of intraocular pressure.
Advantages of ABiC
1- Control the intraocular pressure (IOP) without damaging tissues and without the placement of permanent implants in the eye.
2- Reduce in anti glaucoma eye drops which has the benefit of reducing the cost to the patient and also reduce corneal exposure to preservative ingredients of the eye drops such as benzalkonium chloride (BAK). This ingredient can cause damage to the ocular surface and also many research studies showed that it can induce apoptosis to corneal endothelial cells and also to endothelial cells lining the trabecular meshwork with further damage of the outflow system of the eye.
3- ABiC can be done in phakic and pseudophakic patients or during cataract surgery.
4- It's minimally invasive allowing quicker recovery. The patient can resume normal activities within few days after the treatment.
5- The incidence of postoperation complications are less than that with trabeculectomy and tube shunt.
Indications of ABiC Glaucoma Procedure
ABiC is indicated for the reduction of high intraocular pressure in patients with open-angle glaucoma (OAG) and patients intolerant of anti-glaucoma medications.
Other indications of ABiC:
1. Pigmentary Glaucoma (PG).
2. Pseudoexfoliation Glaucoma (PXF).
3. Ocular Hypertension.
4. Patients after treatment with Selective Laser Trabeculoplasty (SLT).
5. Patients post single session low-power Argon Laser Trabeculoplasty (ALT)
6. Patients with previous failed trabeculectomy or tube shunt surgery.
7. Open Angle Glaucoma with narrow but not occludable angles after laser iridectomy.
8. Normal Tension Glaucoma (NTG).
9. Juvenile Glaucoma.
Contraindication of ABiC Glaucoma Procedure
1. Neovascular Glaucoma.
2. Multiple Argon Laser Trabeculoplasty (ALT).
3. Chronic Uveitis.
4. Chronic Angle Closure Glaucoma.
5. Traumatic/Angle Recession Glaucoma.
6. Narrow inlet with plateau iris.
7. OAG with narrow angle (unless ABiC and phacoemulsification will be done at the same time)
Most common side effects associated with ABiC
1. Intraocular pressure spikes.
2. Hypotony (low intraocular pressure: 5mmHg or less).
3. Bleeding in the eye.
4. Formation of a bleb ABiC Glaucoma
Surgical Steps of ABiC Glaucoma Procedure
1. The eyes will be anesthetized during the procedure.
2. A small incision will be made in the eye at the junction between the cornea and the sclera.
3. A microcatheter will be inserted into the drainage canal.
4. The microcatheter will be advanced around the canal to open the channel and enlarge it.
5. The microcatheter tip is then withdrawn slowly while sterile, viscoelastic gel is injected into the canal to enlarge it to about 2-3 times its normal size.
6. The microcatheter is then withdrawn completely out of the eye.
The intraocular pressure usually drops one to three days after the procedure. It's minimally invasive allowing quicker recovery. The patient can resume normal activities within few days after the treatment.
ABiC has been proven to be clinically effective in reducing the intraocular pressure with high safety profile. Compared to other traditional glaucoma surgeries, ABiC has significantly lower risks. ABiC can be used in conjunction with anti glaucoma eye drops and can be performed after laser or other types of surgery.
ABiC can also be performed with or without cataract surgery. In case the procedure is unsuccessful, other glaucoma treatment options can be used as ABiC does not affect future treatment results.
Regular visits with an eye doctor should be continued as glaucoma treatment is a life-long process.