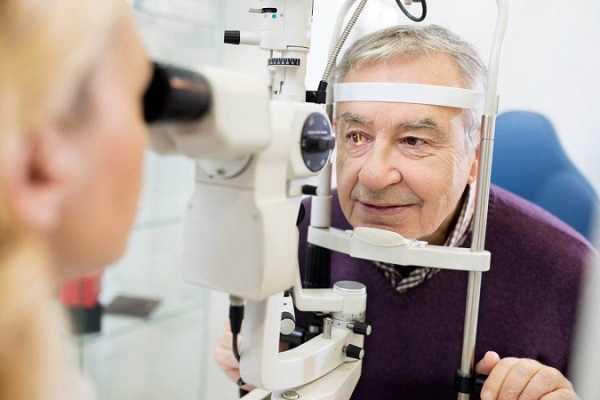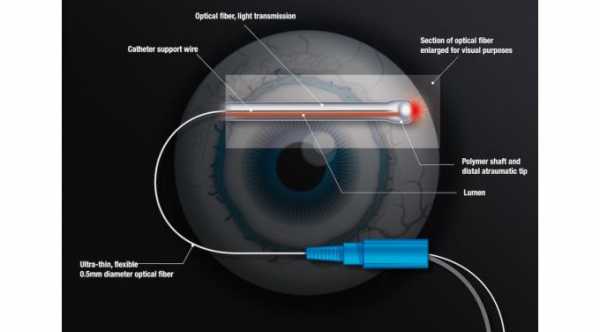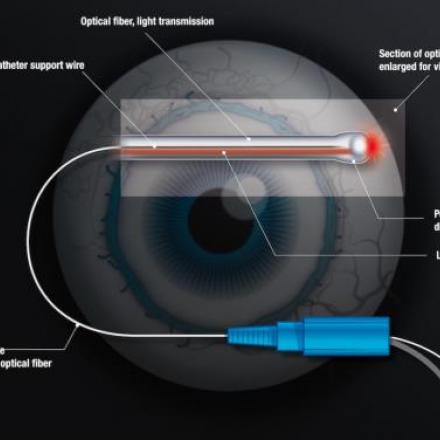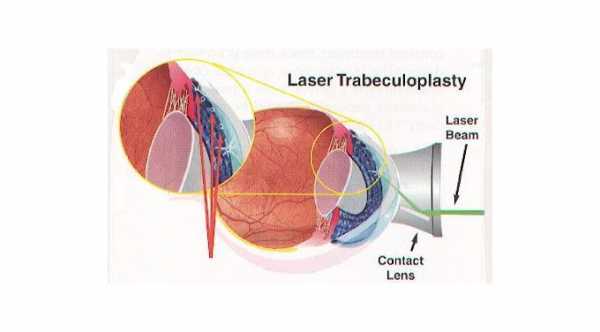
Selective Laser Trabeculoplasty is more effective in eyes with thin cornea
A study confirms that eyes with thin cornea that are treated with SLT ( selective laser trabeculoplasty) demonstrate greater intraocular pressure (IOP) control.
Intraocular pressure is the pressure inside of the eyes that is exerted on the structures, including the walls, of the eyes. Pressure results from the amount of fluids within the eye. These fluids are the aqueous and vitreous humors that are located within closed spaces within the eye. Higher than normal intraocular pressure can lead to glaucoma.
The cornea is the outermost layer of the eye. It is a dome-shaped structure that is clear and covers the front portion of the eye. Although it appears to be a simple clear structure, it is actually made up of a complex group of proteins and cells.
The tissue of the cornea is made up of five unique layers. These layers include the epithelium, the Bowman’s layer, the stroma, the Descemet’s membrane, and the endothelium.
Eye conditions such as glaucoma are caused when there is damage to the eye’s optic nerve from high intraocular pressure. When an eye is healthy, a fluid known as aqueous humor circulates properly inside the front part of the eye. A consistent supply of this liquid is available to maintain a constant and healthy eye pressure.
Eyes with glaucoma have aqueous humor that does not flow out of the eye consistently, which causes a buildup of fluid pressure in the eye, which can eventually cause damage to the optic nerve fibers.
For this reason, early treatment is best, and selective laser trabeculoplasty is often used to resolve the condition in order to restore healthy aqueous humor flow out of the eye.
A total of 47 patients participated in the study. In the study, 80 eyes that underwent the selective laser treatment for primary open-angle glaucoma or ocular hypertension were reviewed.
The eyes were divided into two groups, one group included eyes with thin cornea (less than 555 µm) and the other included eyes with corneas 555 µm or thicker. Data was recorded post surgery at 2 weeks, month 3, month 6, month 9, one year, two years, and, finally, at 30 months. The study confirmed that intraocular pressure was significantly better controlled in the group with thin corneas post treatment with SLT.
While eyes with thinner cornea tend to be at higher risk for progression of cataracts, thinner corneas also have a better long-term response to SLT treatment, at least for the 30-month trial period covered by the study.